What is Lyme disease? What does it look like? Could you or a loved one have it? How is it treated? Learn the answers to these questions, and other startling facts about Lyme disease.

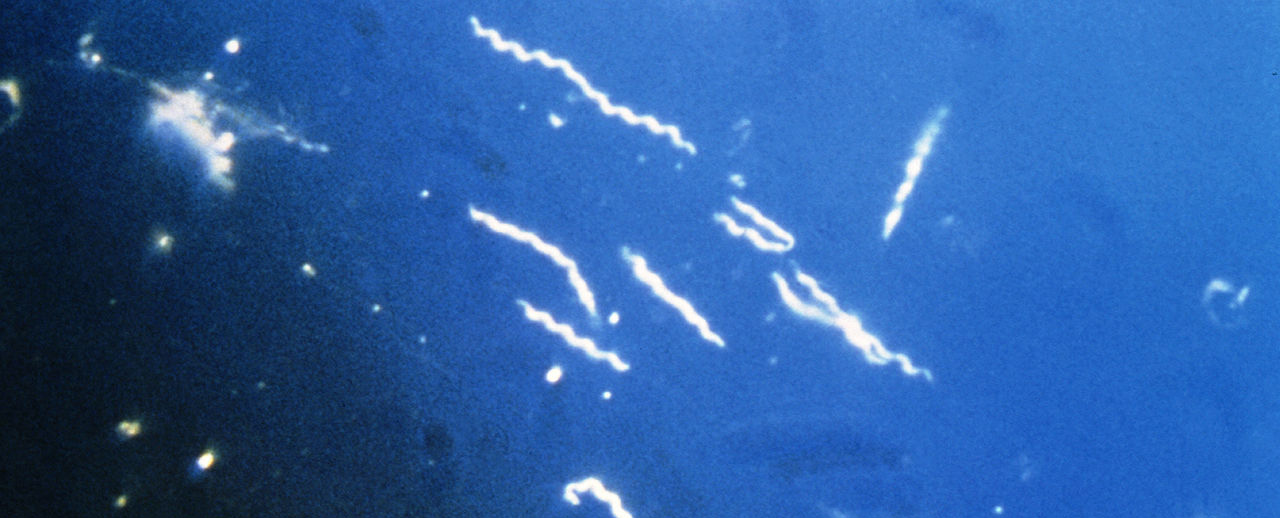
Lyme disease is caused by a spirochete (spiral shaped) bacteria (Borrelia burgdorferi) and is transmitted by certain species of black-legged ticks, as well as the lone star tick commonly found in southern states. The nymphal, or immature, form of the tick, which is about the size of a poppy seed, causes most human cases. Because the bite is painless, many people do not realize they have been bitten. Furthermore, ticks harbor many other diseases that can be transmitted to humans aside from Lyme disease, including other bacterial infections, viruses or parasites. Indeed, there are many diseases (some life-threatening) carried by ticks that can complicate tick-borne disease diagnosis, treatment and recovery, including Babesiosis, Tularemia, Anaplasmosis, Mycoplasma, Ehrlichiosis, Rocky Mountain Spotted Fever, Borrelia miyamotoi, Bartonella, Bourbon Virus, Heartland Virus, Powassan disease among others.
Lyme and tick-borne diseases are prevalent across the entire United States. Fewer than half of patients with Lyme disease recall a tick bite. Likewise, fewer than half of patients with Lyme disease recall any rash. Although the bulls-eye red rash is considered a classic sign and warrants a clinical diagnosis, it is not the most common dermatologic manifestation of early Lyme infection. Atypical forms of this rash are actually far more common.
The Lyme disease bacterium has the ability to enter the brain less than 24 hours after a tick bite. Lyme is called the “great imitator,” because it can mimic ailments such as Multiple Sclerosis (MS), Amyotrophic Lateral Sclerosis (ALS), fibromyalgia, lupus, chronic fatigue syndrome, Parkinson’s, Alzheimer’s, and autism.
Infection with Lyme disease bacteria alone can lead to early symptoms such as severe headaches, debilitating fatigue, joint pain, and skin rashes, while long-term symptoms can lead to problems related to the central nervous system, including the brain, as well as the heart, joints and other musculoskeletal problems. Symptoms of Lyme disease vary for each individual patient, and also vary in intensity over the course of the disease.
Also, check out our Resources for more on Lyme 101, Symptoms, Testing, Finding A Doctor, Pregnancy & Children, Learning & Education, Financial Assistance, Prevention, and Research.
Diagnosis
Did you know that the average patient sees 5 doctors over nearly 2 years before being diagnosed? Or that two-tier testing paradigm for Lyme disease recommended by the Centers for Disease Control (CDC) misses approximately 1/2 of actual cases pursuant to numerous peer reviewed studies? In early infection, CDC endorsed blood tests, which are based on a single Lyme strain from Shelter Island, NY, may not be detecting all the bacterial strains of the disease (there are at least 100 different strains in the United States). According to a Johns Hopkins study, the tests miss up to 70% of infected patients. Without a sufficiently sensitive and reliable test for Lyme disease, it is impossible to determine with certainty who has an active infection versus past exposure. Notwithstanding the unreliability of CDC approved tests, the CDC and FDA have recently taken steps to limit access to more sensitive testing, further compounding the problem. Tick-borne co-infections are also frequently missed using currently available laboratory tests further diminishing the chances of a successful treatment regimen.
Treatment
While those who are able to get promptly diagnosed and treated with antibiotics generally have a better prognosis, there is a significant percentage of patients who are not timely diagnosed or otherwise do not respond to treatment. While the CDC estimates that up to 20% of patients will suffer persistent symptoms after standard Lyme treatment, in a study by researchers at Johns Hopkins University, the treatment failure rate for early Lyme disease was estimated to be as high as 36%. According to another recent Johns Hopkins study, over 63% of patients treated for Lyme disease continue to suffer symptoms that can be debilitating.
There is a deep division within the medical community as to how patients should be treated if they do not respond to a standard course of antibiotics lasting several weeks. There are two evidence based standards of care: International Lyme and Associated Diseases Society (ILADS) and Infectious Diseases Society of America (IDSA).
In recent studies conducted by the CDC, doctors reported using a longer duration than recommended by the IDSA up to 61% of the time, suggesting that such recommended treatments are simply not effective. Moreover, there is a growing body of research demonstrating persistent infection after antibiotic treatment. Lyme patients desperately need more effective treatment options.
Debilitating Symptoms
Infection with Lyme disease bacteria alone can lead to early symptoms such as headaches, fatigue, joint pain, and skin rashes, while long-term symptoms can lead to problems related to the central nervous system, including the brain, as well as the heart, joints and other musculoskeletal problems. Symptoms of Lyme disease vary for each individual patient, and also vary in intensity over the course of the disease. The Lyme disease bacterium has the ability to enter the brain less than 24 hours after a tick bite. Lyme is called the “great imitator,” or the “great masquerader” because it can mimic ailments such as Multiple Sclerosis (MS), Amyotrophic Lateral Sclerosis (ALS), fibromyalgia, lupus, chronic fatigue syndrome, Parkinson’s, Alzheimer’s, and autism.
Chronic Lyme disease may be long lasting, may significantly impair patient quality of life, and may be costly to patients, employers, healthcare systems, and society. In a survey of more than 5,000 patients with chronic Lyme, half report that they have been ill for more than 10 years. These patients suffer a worse quality of life than those with most other chronic illnesses, including congestive heart failure, diabetes, MS and arthritis. Over 43% report that they had to stop working and 25% report that they have been on disability at some point in their illness. They are five times more likely to visit healthcare providers and twice as likely to be seen in emergency rooms compared to the general population.
Research Funding
With neither a reliable test for the diagnosis of Lyme disease, nor an effective treatment for long-term infection, research should be a high priority for this national health crisis. Unfortunately, this is not the case. Although the number of new Lyme cases annually is staggering, there is relatively very meager support for research funding. Indeed, although the annual incidence of Lyme disease is higher than that of breast cancer, hepatitis, colon cancer, Multiple Sclerosis, HIV/AIDS and West Nile virus in the United States, unfortunately federal funding of Lyme disease has been extremely disproportionate. For example, Lyme disease occurs 6 times more often annually than HIV/AIDS, yet it receives less than 1% of the funding from the National Institutes of Health compared to HIV/AIDS. Likewise, there are 141 times as many cases of Lyme disease than West Nile virus, yet Lyme disease receives less than half of the funding for research. Lyme disease has been underfunded far too long. With your help, we can make a change.
So Much More
This is just the beginning of all of the information we have for you on Lyme disease. Visit our Resources for a great deal more on the following: